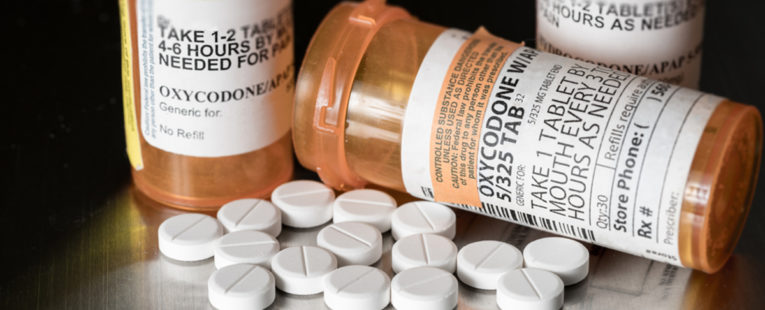
With good intentions, the Joint Commission, which accredits health care organizations across the U.S. declared pain a fifth vital sign in the late 1990s, and made the recommendation that doctors should do whatever they can to ensure patients have no physical discomfort. This includes the prescribing of opiates such as oxycodone, hydrocodone and fentanyl to alleviate pain.
Now, more than 20 years later, the nation faces a growing epidemic of opioid abuse, overdoses and deaths, impacting hundreds of people daily. The crisis has been declared a national Public Health Emergency under federal law and the state of Illinois has developed a special task force to address the problem.
OSF HealthCare is taking a comprehensive approach to deal with this issue with the launch of a Ministry-wide committee overseeing the project. A major initiative of this group includes giving the hospital system the chance to look within itself to understand the prescribing practices of providers throughout the organization.
“It was not part of our process in the past to track opioid prescriptions within OSF HealthCare,” said Jerry Storm, senior vice president of Pharmacy Services. “We didn’t know how often our physicians were prescribing and the amounts patients were taking home. To be part of the solution, we need to understand the opioid prescribing patterns of clinicians as a health care organization.”
As a result, the Healthcare Analytics team, a part of OSF Innovation, has identified data needs and built specific data marts and tools to facilitate and energize the translation of this data into actionable insights. This includes building tools such as the Opioid Explorer, specifically detailing opioid prescriptions within OSF HealthCare. The idea is to give leaders and providers an objective look at prescribing habits.
The Opioid Explorer
The Opioid Explorer breaks the data down into in-patient and out-patient facilities.
“Those using the Explorer can see what’s being prescribed, how many tablets are included in a prescription, how often opiates are given to patients and whether they are administered orally or through an IV,” said Colleen Theisen, a program manager for the Healthcare Analytics team.
This information can be further broken down by region, facility and provider specialty.
“Our providers see hundreds of patients and write hundreds of prescriptions,” said Dr. Richard Ginnetti, regional medical director in the Eastern Region in Bloomington and part of the overall OSF HealthCare opioid initiative. “The Opioid Explorer allows them to view their overall prescribing habits, how that compares to their peers and enables them to provide the best and safest care possible for our patients.”
The overview also gives leaders the information they need to identify providers who may prescribe opioids at a higher rate than others. They could then connect with those physicians and other clinicians for education on appropriate opioid prescription guidelines developed by the Centers for Disease Control and Prevention.
“If you have a particular surgery and we typically sent you home with 30 pills, we might just send you with ten this time around,” said Cheryl Crowe, director of Behavioral Health Services and a member of the overall OSF HealthCare opioid initiative. “Our goal is to send you home with the appropriate amount of medication to help you manage your pain, and reduce the amount of unneeded medication which could just end up sitting in your home, which is a safety risk.”
A combination of efforts, including Ministry-wide education on the appropriate use of pain medications, standardizing opioid prescriptions within the electronic medical record and use of the Opioid Explorer have made difference. In a year and a half, OSF HealthCare reduced tablets per prescription by 5%. The number of opioid prescriptions decreased by 13% and overall tablets were down by 16%.
The fight is far from over
Just as it took more than 20 years for the opioid crisis to surface, it’s going to take time before real progress is made.
“As we have used the Opioid Explorer, we have found that there are more metrics we’d like to include that would enable us to target patients at high risk for substance abuse problems,” said Dr. Ginnetti. “We can then work with those patients on changing medications or using alternative methods for control of pain.”
Other projects the OSF HealthCare Opioid Committee is working on includes the development of better education for patients on reasonable pain expectations and creating care packages with tools for pain management. There are efforts to expand the use of certain drugs used for the treatment of opioid addiction such as Vivitrol and Buprenorphine, and finding ways to partner with the criminal justice system and community agencies such as crisis centers to help those struggling with addiction.
The latest initiative offered is the drug take back program where secure disposal boxes are installed at each of OSF HealthCare hospitals in Illinois and Michigan for people to safely dispose of their medications. About 1.6 tons of drugs have been collected throughout the Ministry in six months.
“All national data indicates about more than 60% of patients who end up having opioid disorders initially start with obtaining tablets left over in a medicine cabinet of a friend or family member,” said Storm. “This is an easy way to reduce the amount of opioids in our communities that could be diverted, misused and abused.”
It should be noted that OSF HealthCare is not trying to get rid of opioids for all patients; however, the health care system does want to make sure opioids are prescribed in the safest, most evidence-based manner that doesn’t put patients and the community at-risk. OSF is making sure it continues to meet patients’ needs for pain management.
The collaborative effort to reduce the amount of opioids in OSF HealthCare communities is just one way multidisciplinary teams come together to build solutions for health care problems.
Last Updated: January 27, 2022